After trying to become pregnant without success, many women make the decision to visit a fertility center for assistance conceiving. If you are reading this, you may be one of them. At GENESIS we know how big this leap can be. We are here to relieve your stress by briefly describing two common ways we can help you become pregnant.
You may have already heard about the two most common and effective treatment options used in reproductive medicine: intrauterine insemination (IUI) and in-vitro fertilization (IVF). How do you know which one is right for you? Below, we explain the difference between IVF vs IUI, how we decide which treatment will best suit your situation and how each treatment compares in terms of timeline, cost and success rates.
Initial Consultation
GENESIS considers patients like family, and we believe family always comes first. This is why you should leave plenty of time for your first visit. Although many of our patients have had some prior evaluation, the initial consultation will usually involve taking a detailed history, then discussing the fertility testing you will need to complete in order for us to establish a diagnosis. There are many causes of infertility and your treatment is tailored to the underlying cause of your difficulty. During your visit, we take the time to answer your questions and to relieve any anxiety you may have about the process of fertility care.
Your first visit is completed by one of our physicians or nurse practitioners. You can choose your practitioner under the Medical Team Tab. Seeing a nurse practitioner is a way to expedite your initial visit. Your follow-up consultation, to review the results of your testing, will be with the physician of your choice. We have found that first establishing a relationship with the nurse practitioner helps keep our patients closely connected and engaged in the care process.
Fertility Testing
Fertility testing is the first step in determining which treatment method is most likely to help you become pregnant. Depending on your history, we will request that you and your partner (if applicable) complete blood tests, sperm analysis and transvaginal ultrasound. In order to decide the best treatment option for you, it is vital we know your:
- genetic history
- menstrual cycle history
- egg quantity
- whether your uterus and fallopian tubes are functioning properly
- and your overall health.
Fortunately, the typical fertility assessment does not take long. Testing is usually complete within four to six weeks, depending on the stage of your cycle when you come in for your first visit. Decisions about treatment can generally be made at the follow up visit with your doctor.
The Differences Between IUI and IVF
IUI and IVF are the most utilized fertility treatments in modern fertility medicine. Although the two treatments are very different, they often get confused with one another. This is often a source of unnecessary stress for patients. Here we will try to relieve the confusion.
Understanding IUI
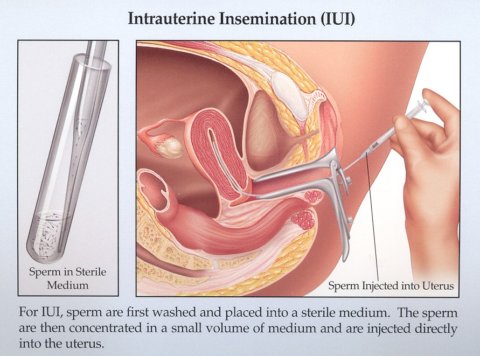
IUI is commonly referred to as artificial insemination. Sperm is inserted directly into the uterus to help facilitate pregnancy. An IUI bypasses the cervix and places sperm closer to your fallopian tubes around the time of ovulation so that sperm can more easily meet the egg. This simple procedure is completed by our nursing staff, and is often carried out together with fertility medications.
An IUI is recommended when there are issues with cervical mucus production, ejaculatory dysfunction or sexual difficulties. IUI is also used for patients in same-sex relationships using donor sperm. It is often used as an addition to other interventions such as ovulation induction. IUI is also recommended as a first step for couples if there is a mildly depressed sperm count or for couples who have been diagnosed with unexplained infertility.
Before an IUI, sperm cells are separated from the seminal fluid (a procedure called “sperm washing”). This takes about an hour. However, the actual insemination takes only a few minutes and usually involves minimal discomfort, if any.
Understanding IVF
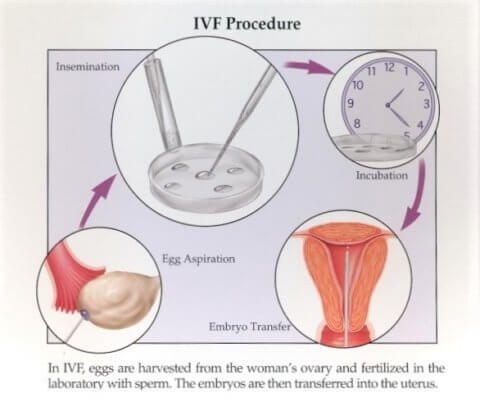
IVF is the process of combining sperm and eggs in a laboratory dish (also called a petri dish) in order to create a fertilized egg, or embryo. Natural, fertility-enhancing hormones are used to stimulate the ovaries to mature multiple eggs. This is possible because, in the natural cycle, many eggs will begin to mature but only one is actually chosen to ovulate. The rest are lost to a process called atresia, or cell death. Natural hormones can rescue some of the eggs that would have been lost to this process and allow them to mature. Multiple eggs can then be extracted and used to create embryos. During this process you will be closely monitored with blood tests and sonograms to assess the development of the eggs in your ovaries and to optimize the time of egg retrieval.
Take the Next Step – Schedule an Appointment
Egg Retrieval and Transfer
Eggs are removed from the ovaries during a procedure referred to as “transvaginal egg retrieval.” This is a procedure that is performed under sedation and generally takes between 15 and 20 minutes. There are no incisions involved and the recuperation is usually fast (but you will have to miss one day of work for this procedure). Prepared sperm from the partner (or, if indicated, a donor) are then used to fertilize the eggs in a laboratory dish by one of our trained embryologists who then closely monitors the development of the embryos. This process takes up to five or six days. Once developed, an embryo is transferred into the uterus where, when successful, it will implant and develop into a fetus and, hopefully, into a healthy baby.
The embryo transfer procedure is nearly identical to IUI but can only be done by a physician. There are many variations in how IVF is done. For example, many IVF treatments will result in cryopreservation (freezing) of the embryos and transfer of a single embryo in a subsequent cycle. The type of IVF that might be recommended for any individual patient will depend on her reason for needing IVF in the first place; as well as her ultimate family planning goals.
IVF is commonly used by women whose fallopian tubes are blocked and for those whose partners have significant sperm anomalies. IVF also has successful outcomes for those who have unexplained infertility, endometriosis, recurrent pregnancy loss and age-related infertility.
Timeline Differences
IUI must be done during the mid-cycle ovulation. Consequently, patients can potentially become pregnant within one cycle, or one month of the treatment. We typically allow patients to complete a maximum of three to six cycles of IUI, depending on her age. This is because the statistical chance of conception is about the same during each of the initial tries. When IUI is not successful over time, the effectiveness of additional cycles begins to significantly decrease. This is likely because there are other factors preventing success. We generally encourage patients in such situations to move forward with IVF.
You can check out the IUI Journey here.
Because IVF requires more complex preparation, the lead time to an IVF cycle is typically one month. The actual time for stimulation ahead of egg retrieval is generally 10-14 days. If fresh embryo transfer is done, the results will be known two weeks later. However, when embryos are cryopreserved, they may be used for transfer – generally one at each attempt – during the following cycle or many months afterwards. Couples who conceive on their initial attempt often return a year or two later. Many then have a successful transfer of a frozen embryo for their subsequent pregnancy
You can check out the IVF Journey here.
IVF vs IUI: Which is more successful?
It is important to note that neither IUI nor IVF can reliably result in a successful pregnancy with every try. Just like couples who conceive naturally with no assistance, these treatments may require repetitive tries until success occurs. Your caregivers can explain the reasons for this as well as the time frame during which you can expect pregnancy to occur. Your fertility assessment will tell us what treatment is most appropriate to start with.
IVF has the highest pregnancy rate per cycle of treatment, but that does not make it the always-preferable choice. IUI is less complex, less invasive, less expensive and more likely to be covered by insurance. There is no reason to choose IVF as a preliminary treatment if IUI has a reasonable chance of working. On the other hand, patients whose situation requires IVF sometimes choose IUI for the very same reasons, in addition to their fears and anxiety.
Choosing treatments based solely on cost can take a large toll not only on your finances, but also on your emotional well-being. Our physicians can give you a general estimate of the success rate you can expect with each option. They can also advise you of the potential risks and complications involved with both treatments. By explaining and demystifying the process of IVF vs IUI, you can better understand the realistic options that you have.
Which treatment increases your chance of multiple babies?
The risk of twins with an IUI is related to the treatment cycle you are using and your age. It has been generally accepted that, when IUI is combined with fertility medications such as Clomid® or Letrozole®, ® the risk of twins is ~5%. This risk increases to 10% – 15% with the use of injectable gonadotropins (i.e. natural hormones). If you and your doctor decide that a natural cycle without drugs is best (including if a “trigger shot” is used), you will not increase your risk of twins. Furthermore, the use of careful monitoring and cancellation of cycles that result in multiple eggs will vastly decrease the risk of multiples.
At one time, IVF was renowned for creating multiple pregnancies. Using elective single embryo transfer has brought the risk of twins down from 30% to ~5% and the risk of triplets or more to <1%. Patients contemplating IVF may therefore be surprised that IVF has actually earned its reputation as the best way to prevent multifetal pregnancy.
The difference in cost
At GENESIS, we understand that cost can be a major factor in the type of fertility treatment you choose. Our financial consultants are onsite and easily accessible to help you navigate your insurance company’s policy and cost of treatment. Paying out of pocket, without any insurance coverage, is always daunting. However, for reasons explained above, the least expensive option may end up being more expensive if all it does is lead to multiple treatment failures. This is the reason that, after a long and difficult effort, GENESIS was excited to be a big part in New York State’s mandate for IVF coverage.
Which treatment option is right for you?
To establish which treatment option is right for you, it is a good idea to talk through your options with a fertility specialist. They will be able to assess your situation and determine whether IVF or IUI would be more appropriate for you.
Sometimes health insurance carriers require multiple rounds of medicated IUI cycles before they will authorize coverage for IVF. Coverage for infertility treatment vary from plan to plan and company to company. With this in mind, each patient is encouraged to research his or her plan coverage extensively in advance, either online or by calling the insurer or benefits representative, or both. Of course, our financial counselors are there to assist you as needed.
At GENESIS every member of our team is committed to helping you through your fertility journey. As you will see, we will be there to assist you at each step along the way.
Original post July 1, 2020
Updated November 9, 2022
If you would like to learn more about GENESIS Fertility New York or are ready to schedule an appointment, please speak with one of our representatives at 929-605-5467.